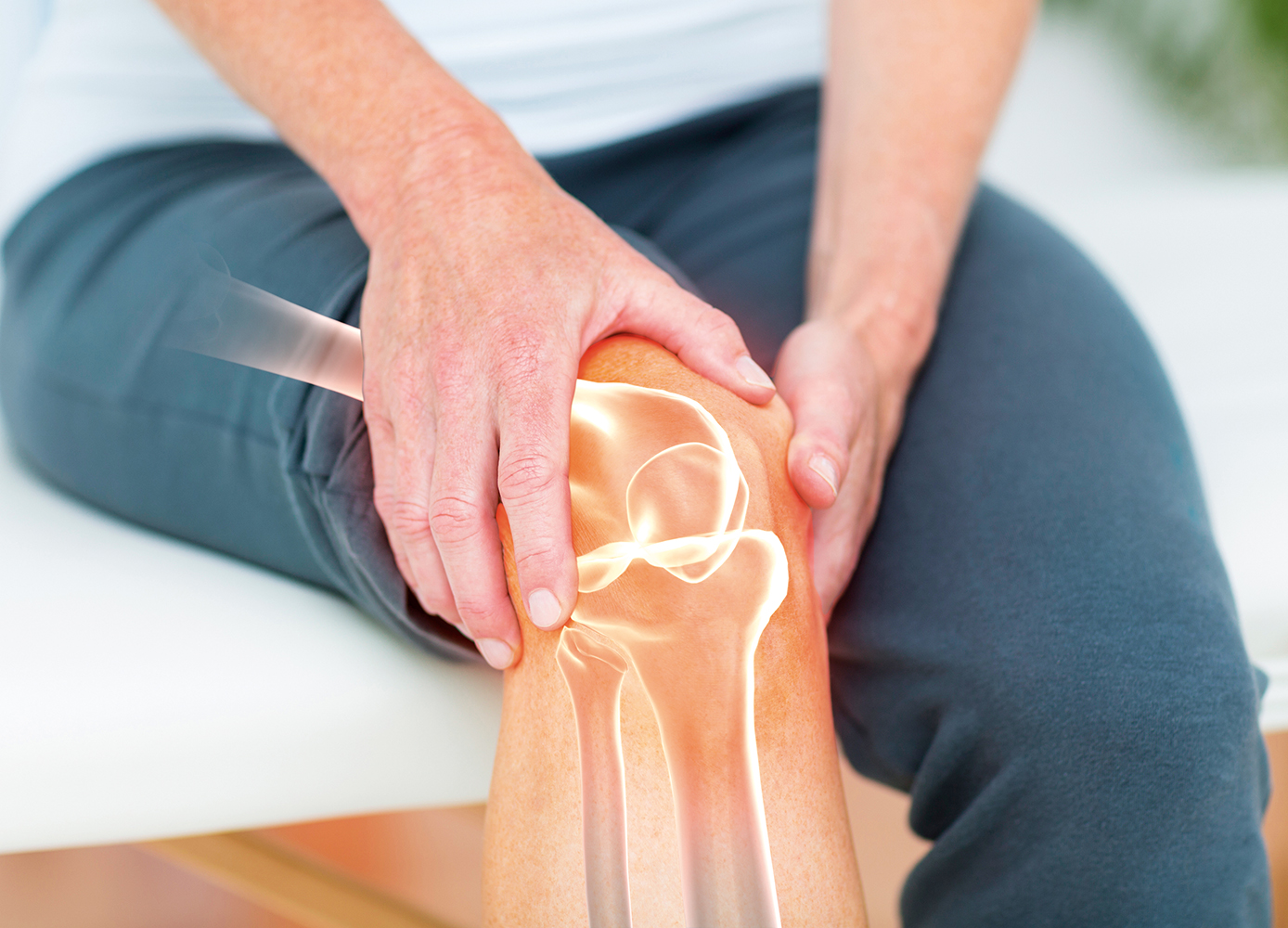
Knee pain may be benign, but it could be a sign of osteoarthritis
A new feature in Good Times magazine is “Your Health Questions,” in which we find experts to answers questions submitted by our readers about health, nutrition and well-being.
By Wendy Haaf
Q. My doctor once told me that the sharp, sudden pains in my right knee were “joint mice” and said that there wasn’t really anything that could be done. The problem went away for decades, but the mice are back. What are joint mice?
A. “Joint mice” is a historical term used to describe loose fragments of bone, cartilage, or both floating inside the knee joint, usually due to a disorder called osteochondritis dissecans (OD). In this condition, which is most common in young people, a section of the cushioning cartilage inside the knee softens or cracks for reasons that aren’t fully understood. Suspects include an inadequate blood supply and multiple traumas.
In its mildest form, “you might get a little bit of softening of the cartilage,” explains Dr. Devin Peterson, an associate professor in the department of surgery at McMaster University in Hamilton, ON. “At the far end of the spectrum, this little piece of cartilage and bone actually breaks off.” Treatment for OD varies from watchful waiting to arthroscopic surgery.
“Sometimes it resolves by itself,” notes Dr. Tom Appleton, a rheumatologist, assistant professor, and scientist with the Schulich School of Medicine & Dentistry at Western University in London, ON. “If it’s more severe and causing an inflammatory reaction, sometimes joint injection or removal of the debris is required.”
You don’t say in your letter whether you have any other symptoms, but just because you’re having pains similar to those you experienced long ago doesn’t necessarily mean that your mice have returned. While OD can happen after age 55, in this age group, knee pain is far more likely to be due to osteoarthritis (OA), a degenerative condition that causes cartilage breakdown. (OA was once believed to be due solely to wear and tear; more recently, it’s become clear that low-grade inflammation is involved.) Either way, it’s a good idea to see a doctor with expertise in diagnosing disorders of the muscles and skeleton, such as a family doctor with sports medicine training, a rheumatologist, or an orthopaedic surgeon, who should be able to figure out what’s going on, based mainly on your symptoms and a physical examination.
“If there’s a problem, you should certainly get it attended to and not ignore it,” Appleton stresses, in part to rule out other possible causes. If it turns out that you have knee osteoarthritis, “we know that exercise is absolutely one of the most effective things to manage the symptoms,” he adds. For one thing, strengthening the muscles around the joint eases stress on the knee. Here too, at least initially, expert guidance is helpful—your doctor can refer you to a physiotherapist or specialized group exercise program, one example being classes offered through GLA:D (Good Life with osteoArthritis: Denmark) Canada.
“There are several medical and non-medical approaches to improve symptoms in knee OA,” Appleton says, but unfortunately, “often people ignore the symptoms or don’t receive evidence-based treatments.”
Unfortunately, we can answer only those letters selected for publication. Write to:
Your Health Questions
Good Times
4475 Frontenac
Montreal, QC H2H 2S2
E-mail: goodtimes@bayardcanada.com
Photo: iStock/Wavebreakmedia.