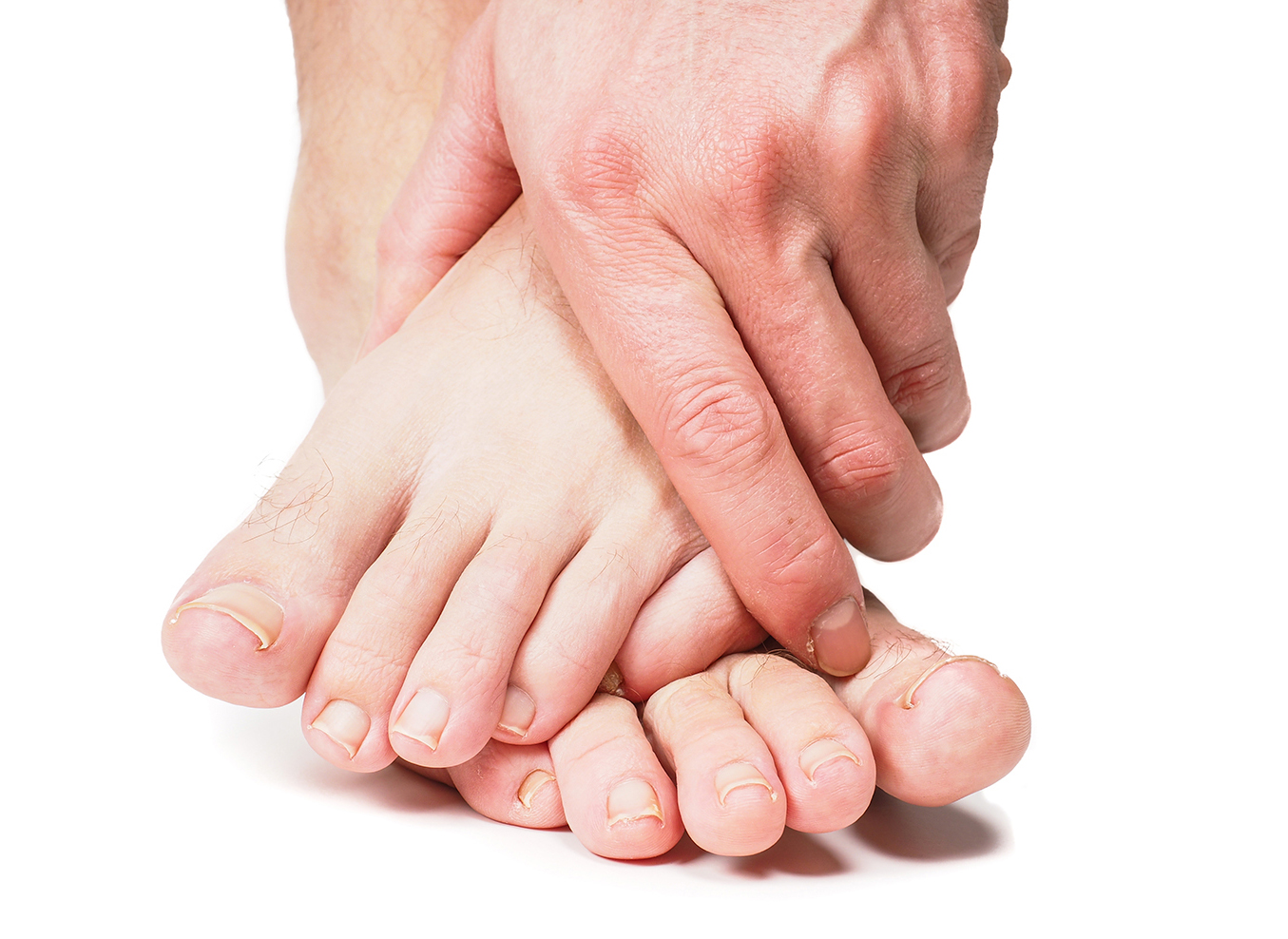
Bunions, corns, calluses, pain…you don’t have to put up with foot problems
By Wendy Haaf
If your feet hurt, it’s hard to stay active, which, as we all know, is key to maintaining good overall health. And even if you’ve never had foot problems in the past, some of the physical changes that occur as we age can make foot problems more likely after age 55. Here’s an overview of some of the common issues that can arise and what can be done to manage them.
Photo: iStock/ArveBettum.
Bunions
If there’s a big bony bump at the base of your big toe and that digit is angled towards the baby toe, you probably have a bunion.
Generally caused by a combination of factors, including genetics (the tendency to develop bunions runs in families) and an imbalance in the muscles that pull across the joint involved, bunions are progressive. Sometimes, a shoe that’s wide and deep enough to accommodate the resulting abnormal shape of the foot (or a shoe that’s been modified to do so) and devices such as spacers, braces, and custom orthotics prescribed by a chiropodist or podiatrist can help decrease discomfort and possibly even slow progression of the bunion.
If such measures fail to offer sufficient relief and you’re otherwise healthy, “maybe it’s time to consider surgery,” says Bradley Sonnema, an Edmonton podiatrist and president of the Canadian Podiatric Medical Association. This can be done by a podiatrist or an orthopaedic surgeon. As with any type of surgery, the operation (there are multiple variations) carries risks, including infection and the possibility that the bunion will eventually return. Nevertheless, according to an analysis of a large number of studies, 85% of patients are satisfied with the results and 10% are somewhat satisfied.
Often a bunion will go hand-in-hand with a hammertoe—the same abnormal biomechanics that cause the former can cause another one of the toes to clench and form a hump. Again, a chiropodist or podiatrist can assess the problem—including factors such as the extent of stiffness in the toe—and try various methods for coaxing the toe into a more comfortable position (for example, with a special splint, a sleeve, or strategically placed padding). In other cases, surgery may be considered.

Photo: iStock/Traimak_Ivan.
Corns and Calluses
“Corns and calluses are the body’s response to repeated pressure or friction,” says Joseph Stern, a podiatrist in Vancouver. Calluses, which appear on the bottom of the foot or on the heel, are flatter and more diffuse, while corns are typically rounded and tend to crop up on the crest of the toe or between the toes.
The resulting thickening of the skin can cause pain. In the case of a callus that suddenly appears on the bottom of the foot, the culprit may be thinning of the fat pad on the sole of the foot, combined with arthritic changes that make the bones more prominent, says John-Paul Gordon, a podiatrist with Body Quest Health & Wellness Centre in St. John’s, NL, and the fix may be as simple as wearing shoes in the house.
You may also be able to prevent heel calluses from becoming dry and thick enough to begin cracking by moisturizing the skin nightly (using a cream containing up to 20% urea) and gently rubbing the area periodically with a pumice stone to remove excess dead skin. Take care not to go too deep with the stone.
A doughnut-shaped non-medicated corn pad may offer temporary relief by shielding the area from further pressure (some practitioners suggest cutting a section out of the pad to form a U shape, thereby preventing a buildup of fluid in the centre of the “doughnut”). Most foot-care providers strongly advise against using medicated pads—the acid they contain can burn and eat through healthy skin, posing a risk for infection.
A chiropodist or podiatrist can painlessly pare away the hardened skin or remove the core of the corn (never perform “bathroom surgery” yourself) and recommend strategies to prevent recurrence. “Often we’ll use padding to offload the pressure,” Sonnema explains, or, “if the corn is between the toes, we’ll use little spacers to keep the toes from rubbing together.”
Heel Pain
If, out of the blue, you start waking up with heel pain that’s at its worst when you first get out of bed, the most likely culprit is a mechanical problem that’s exerting excess stress on the band of tissue stretching along the bottom of the foot from the heel to the base of the toes.
Sometimes the cause is as simple as worn-out shoes, so if it’s been some time since you’ve done so, consider investing in a new pair. In other cases, a simple heel pad or cushion may ease the strain enough to alleviate the pain.
If not, however, consult a chiropodist or podiatrist, who can work through the possible solutions, which may include exercises to stretch too-tight calf muscles and orthotics to correct the mechanics of the foot. For chronic heel pain that doesn’t respond to these methods, surgery to ease the tension on the band of tissue—for example, by lengthening the relevant calf muscle—can offer relief, notes James Hill, a chiropodist and president of the Ontario Podiatric Medical Association.
Ingrown Toenails
When a sharp spike at one of the topmost corners of the toenail (typically on the big toe) begins digging into the nearby soft tissue, that’s termed an “ingrown toenail.”
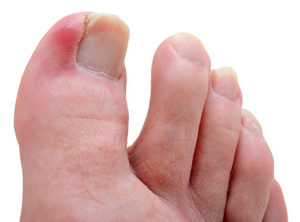
Photo: iStock/kbwills.
“The shape of the nail tends to curve a little bit more as you get older,” Hill says, which is one predisposing factor. To reduce your chances of developing this problem, avoid too-tight shoes and cut your nails in a gentle curve (taking care not to clip them too short) without digging down into the corners.
Caught early—before piercing the skin—some ingrown nails may just need frequent Epsom-salt soaks and a bit of time to grow out. However, if the skin is broken or the area is red and swollen, apply antibiotic ointment, cover lengthwise (as opposed to around the toe) with a bandage, and promptly see your doctor or foot-care professional. If it’s a chronic issue and you don’t have circulation problems, “there are simple procedures we can do that permanently solve it,” Hill says. “We can numb the toe without a lot of discomfort, take out a sliver of the nail, and apply a chemical to kill the root so it doesn’t grow back ingrown. There’s no downtime. I tell my patients that they can go to soccer practice, for example, within hours of the procedure.”
Thickened Nails
Thickening of the nails can be due to poor circulation, trauma (dropping a frozen chicken on your foot, for example), and repeated micro-trauma (for example, from the longest toe repeatedly bumping into the end of the shoe). “If there’s trauma to the nail, the nail can grow back thick and misshapen—just as when you damage the skin, you can get scarring,” Sonnema explains. Thickening can also be a consequence of a fungal infection of the nail.
If you have a thickened nail, it’s a good idea to see a foot specialist, who should be able to differentiate between these possible causes. First of all, fungal infections can spread from one nail to another and they’re notoriously hard to get rid of, even with prescription medications, so the sooner you start treatment, the better. And even a garden-variety thickened nail may worsen without appropriate attention. “Pressure from the thick nail causes more stress on the nail bed, which exacerbates the problem,” says Nadine Webster, president and chief chiropodist at Kawartha Total Foot Care Centre in Bobcaygeon, ON.
For fungal nail problems, topical antifungal medication is one option. If you choose this route, you’ll need to apply the solution daily for eight to 12 months and periodically visit the podiatrist or chiropodist, who will use a special tool to thin the nail (this allows the medication to penetrate more completely). Regular visits for this same procedure can also keep a simple thickened nail from worsening; if that’s too much of a nuisance, you can also opt to have the nail permanently removed.
“A lot of problems can be fixed simply and quickly, particularly if they’re addressed early,” Webster says. “A lot of people don’t understand how we can help,” she adds, noting other patients may be worried that treatment will be uncomfortable. “Then once we treat them,
they’re so surprised and relieved; they leave saying, ‘If only I’d known!’”